Sleep apnoea is a common cause of night time snores and can even lead to insomnia. It is estimated that around 936 million adults worldwide are affected by this condition. Sleep apnoea can pose health risks if not diagnosed and treated in a timely manner and it is important to be aware of common symptoms. Below you will find helpful information on the treatments available, however, please consult your local specialist to ensure you choose the right treatment for your needs.
What is sleep apnoea?
Sleep apnoea is the starting and stopping of breathing while you sleep. The most common form is obstructive sleep apnoea (OSA). If not treated or managed, it can pose a severe health risk.
The severity of an individual’s sleep apnoea is determined using the apnoea hypopnoea index (AHI). An apnoea is when there is an absence of airflow through your nose and mouth for at least 10 seconds. A hypopnoea is when there is a partial collapse of your airway, which limits normal breathing. The AHI measures how many apnoeas and hypopnoeas occur each hour:
- Normal – An AHI reading between 0 to 5 episodes per hour
- Mild OSA – an AHI reading of 5 to 14 episodes per hour
- Moderate OSA – an AHI reading of 15 to 30 episodes per hour
- Severe OSA – an AHI reading of more than 30 episodes per hour
There are two types of sleep apnoea: obstructive sleep apnoea and central sleep apnoea.
Symptoms of sleep apnoea
Sleep apnoea can present itself through a variety of symptoms and hence prove elusive to diagnose. It is vital to be aware of a multitude so you can detect it early and visit your local GP or sleep specialist. Common symptoms of sleep apnoea include:
- Reduced focus
- Morning headaches
- High blood pressure
- Decreased sex drive
- Irritability or frustration
- Excessive daytime sleepiness
- Trouble focusing during the day
- Dry or sore mouth upon awakening
- Increased need to get up from bed to urinate
- Restless sleep with periods of wakefulness during the night
- Loud snoring that is often punctuated by gasping or choking sounds
Causes of sleep apnoea
Sleep apnoea is essentially caused due to the obstruction of airflow. However, it can also occur due to many reasons that we have listed further below. More information on the two types of sleep apnoea:
Obstructive sleep apnoea (OSA) occurs when your upper airway becomes blocked often while you sleep, thus reducing or completely stopping airflow. Anything that could narrow your airway such as large tonsils, or obesity can increase your risk of obstructive sleep apnoea.
Central sleep apnoea (CSA) occurs when your brain fails to send the signals needed to breathe. Health conditions that affect how your brain controls your airway and chest muscles can cause central sleep apnoea.
It is important to remember that OSA is far more common than CSA amongst individuals.
Risk factors for sleep apnoea
Sleep apnoea is often associated due to a number of risk factors. In people with OSA, the airway has narrowed due to many potential factors, including:
Being overweight: excessive body fat increases the bulk of soft tissue in the neck, and can cause strain on the throat muscles; excess stomach fat can also lead to breathing difficulties
Being male: OSA is more common in males than females but the cause is unknown; it may be due to different patterns of body fat distribution
Being 40 years of age or more: although OSA can occur at any age, it’s more common in people who are over 40
Having a large neck: men with a collar size greater than around 43 cm (17 inches) have an increased risk of developing OSA
Menopause (in women): changes in hormone levels during the menopause may cause the throat muscles to relax more
Having a family history of OSA: genes inherited from your parents may make you more susceptible to OSA
Nasal congestion: OSA occurs more often in people with nasal congestion such as a deviated septum
Other risk factors include:
- Taking medicines with a sedative effect
- Having an unusual inner neck structure
- Alcohol
- Smoking
How is sleep apnoea diagnosed?
You can carry out self-assessments at home using:
- Epworth Sleepiness Scale
- STOPBANG Questionnaire
- Keeping a sleep diary
If these self-tests yield a positive result, it is important to visit your local GP for further advice and seek a referral to a sleep specialist.
A sleep specialist would take a detailed history and may perform a physical examination of your airway. A sleep study may also be recommended to allow the specialist to check for sleep apnoea, and determine the severity. Based upon these findings, the sleep specialist would be able to recommend appropriate treatment for you.
Treatments for sleep apnoea
There are 3 key treatments for sleep apnoea:
Lifestyle changes: losing weight, reducing alcohol and smoking can help reduce sleep apnoea symptoms. Sleeping on your side can also reduce sleep apnoea in some cases.
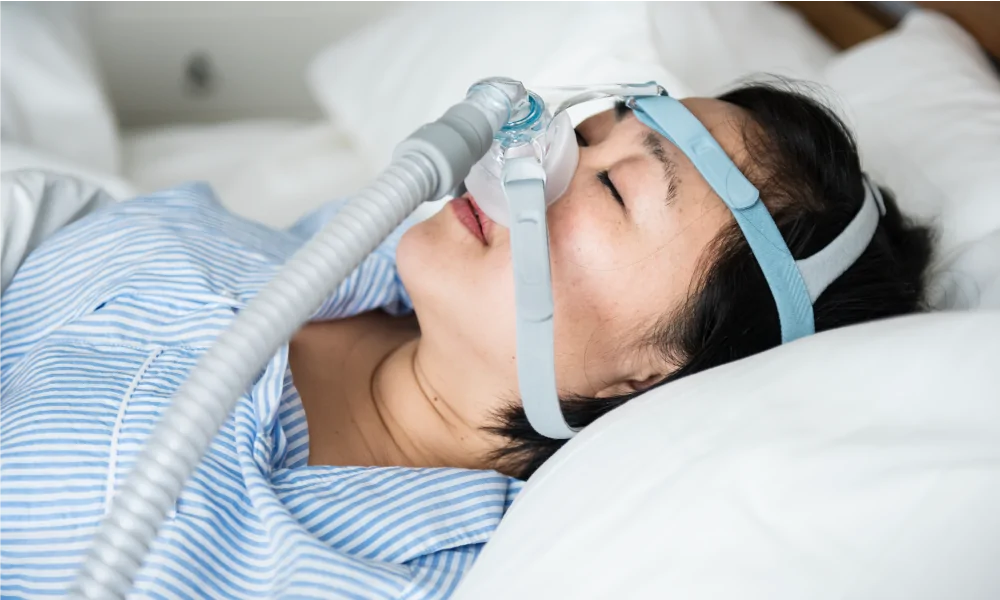
Positive airway pressure therapy (PAP): These devices provide a continuous flow of air into your airways. This stream of pressurised air keeps your airways open and prevents them from closing during sleep.
Mandibular advancement device (MAD): This treatment is unique to every individual. It is a gum shield like device which fits around your teeth and holds your jaw and tongue forward. This increased the space at the back of your throat, thus reducing sleep apnoea symptoms.
Surgery can also be advisable in very severe cases or where the cause of sleep apnoea is determined to be due to be physical in nature e.g. large tonsils. However, in most cases surgery is not the first line treatment.
Sleep apnoea in children
Sleep apnoea can also occur in those younger. Whilst the primary cause in adults is obesity, the primary cause in children is often due to physical barriers such as adenoids or large tonsils. It has been noted that there is a rising prevalence of OSA amongst preschoolers, however, most tend to grow out of this as symptoms and effects are often mild.
The majority of symptoms for sleep apnoea are the same in children, as they are in adults. The key difference to be aware of is that whilst adults experience daytime sleepiness, children are more likely to experience behavioural difficulties.
COMISA
COMISA is the co-occurrence of sleep apnoea and insomnia in an individual. COMISA can sometimes be hard to diagnose due to the overlap of symptoms between sleep apnoea and insomnia. COMISA has been reported to be associated with an increased risk of hypertension and cardiovascular disease.
If you suspect that you are showing symptoms of either one of the conditions then I would urge you to get in touch with your local GP or local sleep specialist. It is critical to receive a timely diagnosis and commence treatment to ensure you are looked after and your risk of developing further health conditions is reduced.
Living with sleep apnoea
Sleep apnoea can be a debilitating condition for many individuals. It is of paramount importance that the right steps are taken to ensure you receive the best care and treatment.
As a leading sleep psychiatrist we have partnered with the best sleep apnoea physicians to ensure my patients receive the right care for them. One such sleep expert is Mr Vik Veer, a leading ENT surgeon and sleep specialist. For further information on sleep apnoea please visit his YouTube channel or website.
If you suspect that you may be suffering from insomnia or COMISA, please do not hesitate to get in touch.